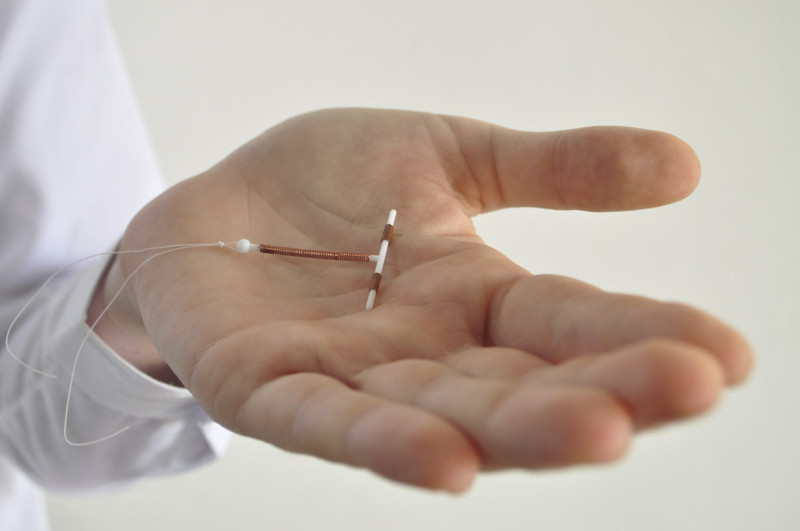
"Providers were much more likely to counsel them on these highly effective methods -- IUDs and implants," said UCSF Prof. Cynthia Harper, lead author of the study. "Women had demonstrated greater knowledge of these methods. They were more likely to select them."
Harper says that there have been new methods that have come out in the last few years, including the hormonal IUD and the contraceptive implant. The training helped clinicians to understand technicalities about each method, including their benefits, side effects, and who was most appropriate for each.
In the study, UCSF partnered with 40 Planned Parenthood clinics in 15 states, including California. Workers at half the clinics received training about birth control methods; half did not.
The discussion of IUDs and implants was starkly different between the clinics that received the counseling and those that did not: 71 percent of providers who received training discussed them versus 39 percent in the control group.
Fifteen-hundred women, ages 18-25 enrolled in the study. They were eligible only if they said they wanted birth control counseling and that they did not want to become pregnant. Those who received counseling with health care workers who had the training chose an IUD or implant 28 percent of the time versus 17 percent of women at the control clinics.
Harper says a major barrier for many women in choosing an IUD or implant was cost. IUDs can cost up to $1,000. But they actually are more cost effective over time, since their effectiveness lasts for years.
The study was done from 2011-2013, before the Affordable Care Act -- and its coverage of birth control -- took full effect, and a38 percent of the women studied did not have health insurance.
"I'm hopeful that if the ACA is in place and if women are more likely to be insured for contraceptives," Harper said, "then they'll be able to afford these methods that have higher upfront costs."
The pregnancy rate dropped from 15 percent to 8 percent over a year. But for reasons the researchers cannot explain, that was only among women seeking family planning services. There was no change in the pregnancy rate among women who sought birth control after an abortion.
The researchers found that fewer women who wanted to use an IUD or implant after an abortion were actually able to get them. Nearly a quarter of these women were pregnant again with a year.
"Forty-four percent of the women who chose (IUD or implants) in abortion care actually obtain them," Harper said. "Now we're looking at why, what were the restrictions." Harper noted that there are restrictions in using public money for birth control in clinics that provide abortions.
The study was published in the Lancet and was funded by the William and Flora Hewlett Foundation