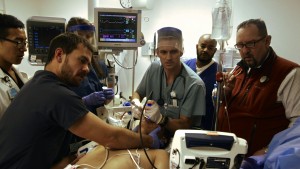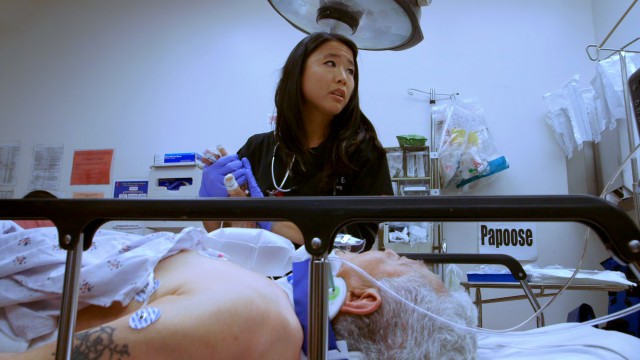
Don't eat a sandwich before you sit down to watch the documentary "Code Black." In one of the first scenes, we watch a team of doctors and nurses cut into a patient. It's a bloody business, and the camera doesn't turn away. That's because this film is about the brilliant chaos of emergency care, and the people drawn to this work.
For all the debate over health care in America, it's relatively rare to hear from doctors on the front lines, and even more rare to hear from young doctors about a field they've recently chosen to devote their lives to. “Code Black,” a documentary by a doctor when he was a resident at LA County's USC Medical Center, delivers that perspective with punch and passion. It promises a look into "America's busiest ER."
Ryan McGarry is now an assistant professor and physician at The Weill Medical College of Cornell University. Possibly, his penchant for storytelling has something to do with his bachelor's degree in English at Pennsylvania State University. His decision to become a doctor was inspired in part by his experience as a Stage IV cancer patient while an undergraduate. Even though he switched gears professionally, he finds poetry in his new field.
His training ground for emergency medicine is “C-Booth”, a now-closed but legendary trauma bay, where “more people have died and more people have been saved than in any other square footage in the United States,” McGarry tells us in his voice over.