Just last September, an analysis by researchers at Kaiser San Francisco found no new HIV infections in over a two-and-a-half-year period among patients who took PrEP.
Ryan McKeel, a spokesman for Gilead Sciences, Truvada's manufacturer, said in an email that "no single intervention is 100 percent effective in preventing HIV. In this case, the individual contracted HIV while taking PrEP due to exposure to a rare strain of HIV that is resistant to both of the drugs included in Truvada."
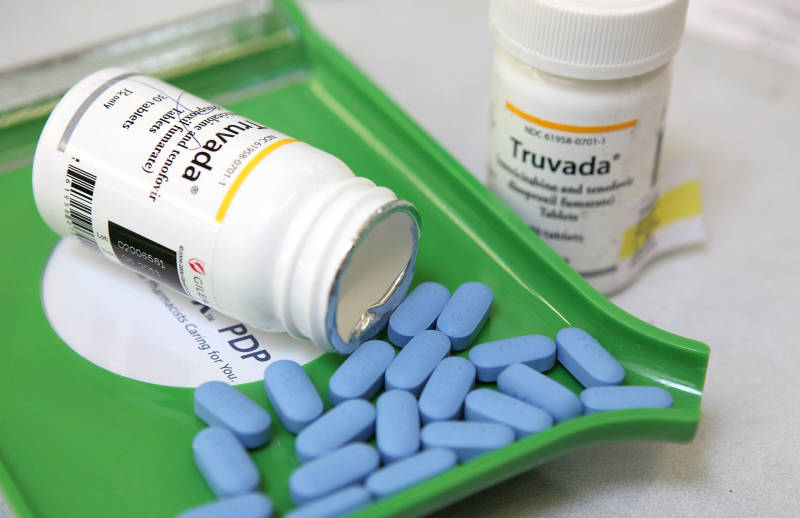
Truvada: The Miracle Drug No One's Taking
Before the FDA approval of PrEP, in 2011, I interviewed the seminal AIDS researcher Dr. Paul Volberding about studies showing Truvada's effectiveness in preventing HIV transmission. He was tremendously excited about the possibilities of a prophylactic drug. "This is the kind of effect we might expect from a very good vaccine," he said.
That enthusiasm has spread to both the Centers for Disease Control and the World Health Organization. CDC now says about 1.2 million people should at least consider PrEP, and four months ago the World Health Organization broadened its recommendation of who should take the medication, from men who have sex with men to "all population groups at substantial risk of HIV infection."
Yet, what some have called a "miracle drug" that works better than condoms has been a bust in terms of adoption by the public.
"Why Is No One On the First Treatment To Prevent H.I.V.?" The New Yorker asked in 2013.
"Why have only 1,774 people—half of whom are women—filled Truvada prescriptions over the last two years?" Slate asked in 2014.
"Gilead’s Pill Can Stop HIV. So Why Does Almost Nobody Take It?" Bloomberg asked in 2015.
"The miracle AIDS drug that people refuse to take," an op-ed headline in The Washington Post read just two months ago.
"Truvada’s been a financial success, bringing Gilead $1.79 billion in the U.S last year," Bloomberg reported in July. But that is due to its use by HIV-positive patients, not in those taking it for prevention. The report cited a study published in the November 2014 Journal of the International AIDS Society that found an unbelievably low 3,253 people, in the U.S., had used Truvada for PrEP between January 2012 and March 2014 -- only about 1,900 of those men.
The CDC says that figure is now about 21,000. According to an October 2015 presentation by Dr. Robert Grant, the protocol chair for a multinational study on PrEP, the number of U.S. users is about 22,000, and use of the drug "has reached a tipping point."
Not according to Michael Weinstein, president of AIDS Healthcare Foundation, a global HIV/AIDS organization. Weinstein has been outspoken against mass adoption of Truvada, arguing it's a poor public health solution and drawing the wrath of some in the HIV health community. (The New York Times' Upshot column called him "the most hated man in the AIDS business" in 2014.)
Weinstein is well aware that the number of people taking Truvada is trivial.
"The bottom line is we are now almost four years since the approval of this, and the last report from the CDC was that 21,000 people were taking it. Really, it's an insignificant number."
He said he thought the recent report about the Truvada failure out of Toronto "will give some people pause" about the drug. And he thinks the focus on Truvada is wrongheaded:
"The messaging coming out is all about Truvada and PrEP, and not about condoms," he said. "So we're seeing this huge spike in STDs across the country. And I think it's because the CDC has really taken their foot off the gas and they're not saying anything about safer sex."
Dana Van Gorder is the executive director of Project Inform, which advocates for new HIV and hepatitis C treatments. He agrees that reduced condom use is a big factor in the rise of STDs. But he says PrEP use is so minimal, it can't be the culprit. Plus PrEP is better.
"Condoms have been a great device, but on a statistical level, they're not as effective as PrEP can be in preventing infections, and the reality is just that not everyone is going to use them, for a variety of different reasons. So it feels unethical to us to not provide people with another option.
"We can't just wish that people are going to use condoms more than they are."
Van Gorder said those who support Truvada were "disappointed" over the news it had failed for someone. But, he said, "We'll continue to encourage PrEP use and stress it is highly effective but not necessarily 100 percent effective."
What, Exactly, is the Problem?
The reasons for PrEP's failure to catch on are manifold, Van Gorder said: Lack of effective education campaigns among people of color and injection drug users, for one; the need for follow-up appontments and testing, for another.
Also, he said, health care providers are not talking enough about PrEP to their patients. Some "are actually hostile to it," he said.
Finally, Van Gorder said, PrEP is expensive. "Covering its cost is not a small matter. While many insurers if not most are covering it, people often have high cost of sharing with deductibles and copays. Not everyone is in a position to [use] it."
But as Lisa Aliferis reported in KQED's State of Health blog last September, there's another reason PrEP has failed to take off:
"Despite the success of PrEP as a preventive, stigma remains," Aliferis wrote. "People who take PrEP are sometimes viewed as promiscuous, [A PrEP patient] told me. “People say, ‘Why are you not just using condoms?’ … Sometimes people say, ‘You must be a slut.’
In fact, the term "Truvada whore" has often been used to describe PrEP users ... and not in a nice way, either. (The term has been co-opted by some Truvada fans.)
The Patient Speaks
Earlier this month, POZ, a magazine for people who are HIV-positive, published an anonymous-yet-candid interview with the Canadian PrEP user who still became infected.
When asked if PrEP altered his sexual behavior or attitudes, he answered:
"Yes. I became more sexually liberated. It took away the fear. I mean, that’s really one of the reasons why people behave themselves [sexually]. It’s not because of morals or religion or society; it’s just the fear of getting sick—especially the fear of HIV. But once you’re on PrEP you’re more comfortable. You feel safer."
He said he's still a fan of the drug, despite its failure.
"PrEP’s a calculated risk," he said. "It’s important for people to know that there is the possibility as opposed to the fantasy that there have been no recorded infections on PrEP. At least now there is one, so it makes it more real."